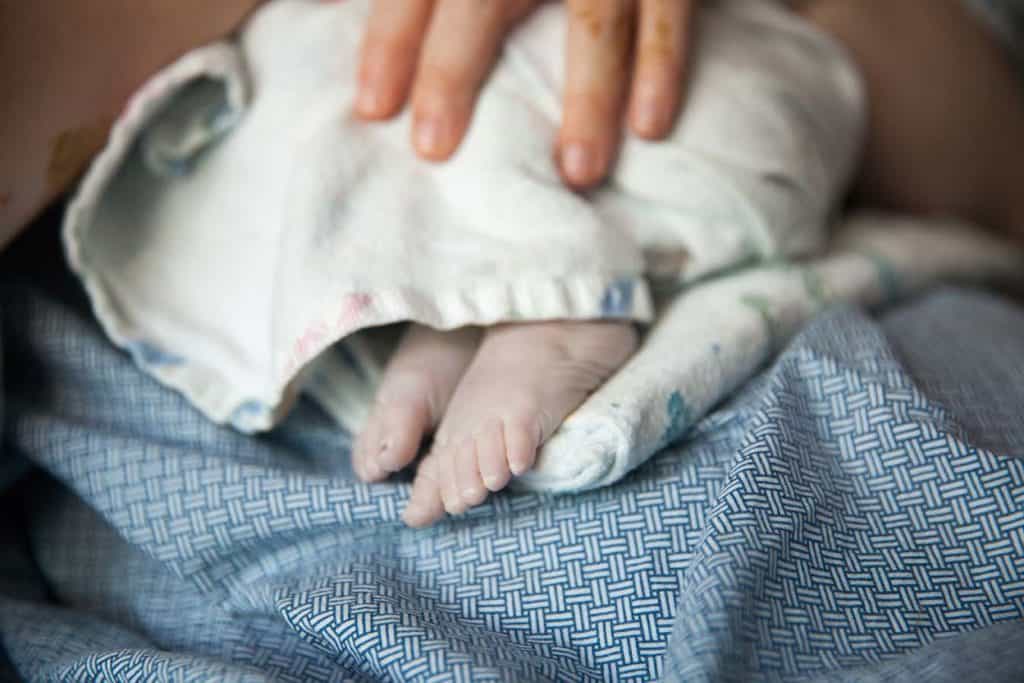
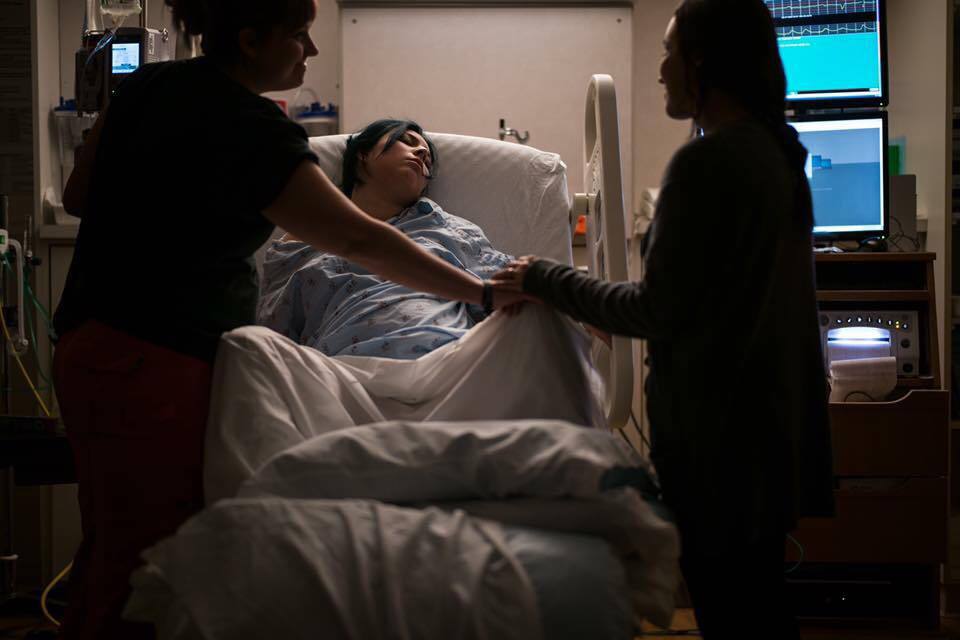Birth Doulas
4 Reasons a Surrogate Needs a Birth Doula
Surrogacy is a beautiful gift to families that have struggled to have a child. There are so many aspects about surrogacy that are planned and thought out from the beginning. One of them can and should be is if the surrogate should have a doula for the birth. As a doula myself, I see the…
Read MoreHow To Have An Empowering Out Of Hospital Birth Transfer (just in case!)
By: Candace Roper Planning for a hospital transfer might seem like the last thing you want to think about when expecting an out of hospital birth. That’s what I thought when I was having my first baby and planning a home birth. Then, at 39 weeks, I found myself giving birth in a hospital,…
Read MoreSpotlight: 2018 UDA Spring Conference Speakers
The Annual Utah Doula Association conference is fast approaching. During this uplifting and educational event, we will hear from several experts on a variety of topics that will enrich and improve our birth-centric businesses. With many opportunities for continuing education credits, tips and tricks for improving our business skills and networking opportunities galore, the 2018…
Read MoreOn Birth, Diversity, and “The Last Man on Earth”
It was just after 8 o’clock. We finally got the kids down to sleep after a long, chaotic day, and I decided it was time to unwind with a mindless episode of The Last Man on Earth. Do you know it? In a nutshell, it’s a comedic tale of a rag-tag group of people who…
Read MorePerinatal Mood and Anxiety Disorder (PMADs) and Seasonal Affective Disorder (SAD) – Holiday Delight
Perinatal Mood and Anxiety Disorder (PMADs) and Seasonal Affective Disorder (SAD) PMAD (Perinatal Mood and Anxiety Disorder) is the name for a range of emotional and physiological responses to pregnancy and childbirth. SAD (Seasonal Affective Disorder) is a type of depression that comes with the change in the seasons. Usually the symptoms will start in…
Read MoreLoving your postpartum body
Loving your postpartum body It was 2011 and I was pregnant with my first child. Every week was exciting as I watched my body go through this incredible transformation. It was so crazy to physically see my body grow…
Read MoreWhat feeding a newborn really looks like
What feeding a newborn really looks like Expectant parents often daydream of the little fingers and little toes that will be joining their family in the coming weeks or months. Daydreaming, for most expectant parents, will also include things like diaper bags, baby carriers, and feeding. We plan, we study, and we prepare for what…
Read MoreKnow Your Birth Options
By Sheri Rysdam To those giving birth, and the people who support them—you’ve got options! As a birth worker, I am often surprised by how *infrequently* people ask for advice, options, and perspectives about childbirth. If you’re reading this, you’re probably the exception. You’re likely either a birth worker or soon to be giving birth,…
Read MoreLying In with Your Baby: The First Two Weeks – Fiona Judd
Lying In with Your Baby: The First Two Weeks – Fiona Judd We’ve all seen her—the mom who has her baby and two days later is back in the grind of carpools, shopping, and even laundry. We wonder how she does it. We secretly hope it happens to us. Our culture seems to value women…
Read MoreThe Call to Build Villages
The Call to Build Villages by Tresa Haymond (VillageWITH.com) The day I heard about Emily Dyches’ tragic death was the moment I felt a call to do something. As I sat sobbing on the edge of my bed, I felt a powerful force connecting my heart to Emily’s heart, as if I knew her well. This…
Read More