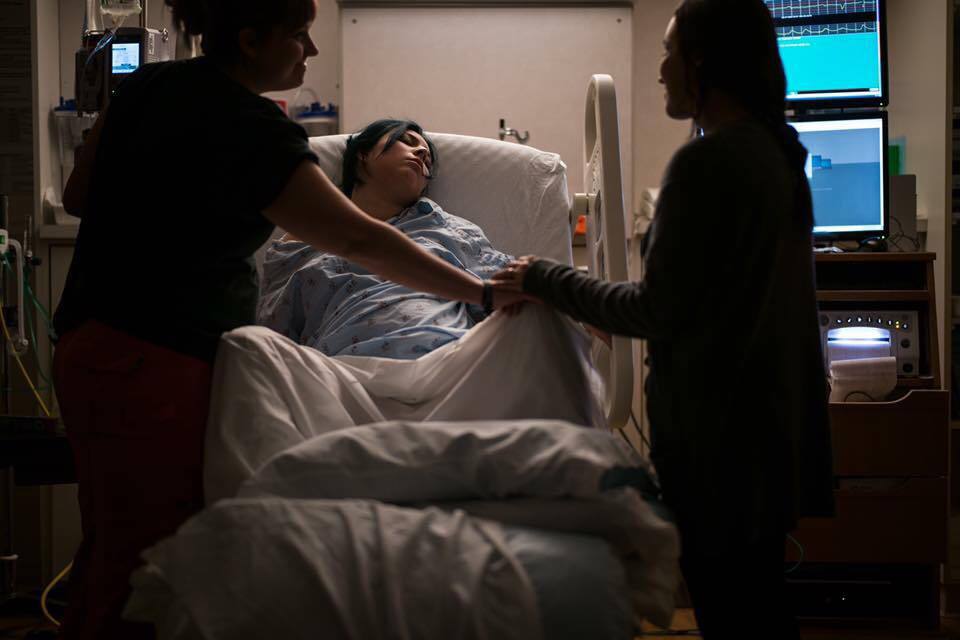Posts Tagged ‘Childbirth’
4 Reasons a Surrogate Needs a Birth Doula
Surrogacy is a beautiful gift to families that have struggled to have a child. There are so many aspects about surrogacy that are planned and thought out from the beginning. One of them can and should be is if the surrogate should have a doula for the birth. As a doula myself, I see the…
Read MoreHonoring the Postpartum Period After Loss
By: Raquel Alfaro For any family, the postpartum period is a time of adjustment and change. Sleepless nights and demanding days. It is no less so for you parents experiencing the loss of a pregnancy, the loss of your baby. It is compounded by not only dealing with the changes of the postpartum period, but…
Read MoreChallenges in Childbirth: What You Need to Know About Trauma and Military Veterans
Guest post by UDA Vice-President Rachel Winsley Most people in our community know that I am a combat veteran, and have worked to support women in childbirth, breastfeeding, and peaceful parenting for many years. What you may not know is that I am also someone diagnosed with Post Traumatic Stress Disorder (PTSD) and Military Sexual…
Read More